– Dr Shivangi Gajwani Jain
Introduction
Although direct resin composites are the most common restorative option for missing tooth structure, the indirect composite restorative techniques are still not our go to option in many practices. The indirect composites, used to rehabilitate large defects owing to decay or fracture of the tooth help the clinician to overcome practical issues such as time management, difficulty in building the occlusal anatomy and tight proximal contacts. In theory, the indirect way should also reduce polymerization shrinkage, micro leakage and color instability in comparison with the direct composite restorations, though further long term studies are needed.
Case Report
A 48 year old male patient visited our practice with a chief complaint of sensitivity and difficulty in chewing hard food. On clinical examination it was observed that all four cusps needed build up while there was no pulpal involvement. Due to the need for complete occlusal coverage, an indirect restoration was planned and composite was the material chosen.
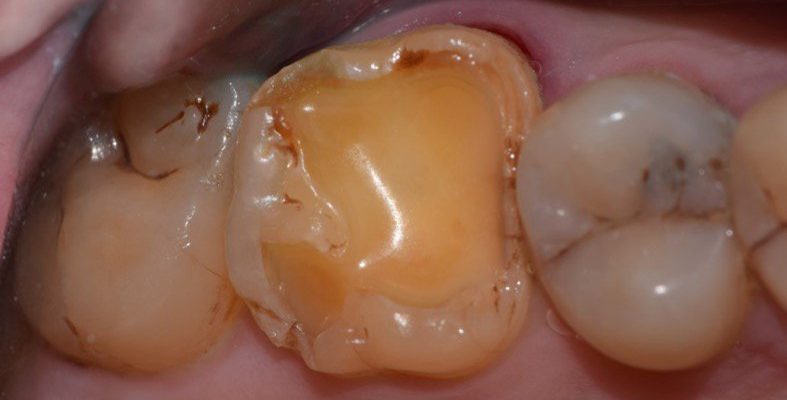
Fig 1. Pre operative clinical picture, occlusal view

Fig 2. Preoperative clinical picture, buccal view showing food lodgment

It was decided to fabricate an indirect restoration in the clinic and bond to the prepared tooth at the same appointment to reduce the number of sittings and cost to the patient.
Onlay tooth preparation – We began with anesthetizing the tooth. The undermined enamel and the proximal caries were removed as we achieved a 360 degree enamel margin for enhanced bonding. The clinical tooth height was 6 mm, and an occlusal clearance of 2mm on the non functional cusps, and of 2.5 mm on the functional cusps was achieved. The proximal contacts were broken. The margins were placed supragingivally, away from the gingival zenith by 3 mm (buccally) and 2 mm (palatally & proximally).
Fig 3. Cuspal reduction with a clearance of 2-2.5mm

Indirect restoration fabrication – Post the onlay preparation, an alginate impression was made and poured immediately in die stone to retain all the details. Once the stone was set, a dye separator (Shofu Dental) was painted on the cast to ensure that the resin does not stick to the dye.
Fig 4. Alginate impression of the prepared tooth

Fig 5 Impression poured in Dye

A light cured composite resin (Ivoclar Vivadent), was used to build the onlay in an incremental fashion and each layer was cured for 20 secs with a curing light (3M). In the final composite layer dark brown tints (Color plus, Kerr) were used to mimic pits and fissures of a natural tooth. Composite complete coverage restoration was fabricated and removed from the dye. Then the intaglio surface was further cured for 60 secs to minimize shrinkage.
Onlay conditioning & Bonding protocol – Once the restoration was ready, the patient was seated, and the tooth prepared for bonding. Heavy rubber dam sheet placed for isolation and the indirect composite onlay checked for fit and marginal integrity.
Fig 6. Heavy rubber dam sheet placed for isolation

Fig 7 Wedges placed

Once checked, the intaglio surface of the onlay was air abraded by 50 microns alumina particles, washed, conditioned with 35% phosphoric acid gel (Ultra etch, Ultradent) and placed in an ultrasonic bath for two minutes for cleansing.
Meanwhile, on the prepared tooth selective etching was done and after a thorough wash, an adhesive and dual cure luting resin was used (Multilink N system by Ivoclar Vivadent) for bonding the onlay. Initial tack curing was done to facilitate excess removal and then cured for 20 seconds on each surface. Water soluble glycerin jelly was applied to prevent oxidation inhibition. Post rubber dam removal, occlusion was adjusted, contacts rechecked and the final finishing and polishing done by wheels (eve diacomp plus twist polishers).
Fig 8. Multilink N system used for bonding

Fig 9. Onlay bonded to the tooth

Fig 10. Final view

Discussion
Indirect restorations chairside or laboratory fabricated are a viable treatment option when a large defect is present. Severely affected occlusal anatomy such as two or more missing/decayed cusps and affected contacts can be restored with predictability as the restoration is created extra-orally.
Crown Vs Onlays: According to various studies, certain factors affect the success of the indirect partial coverage restorations which need to be considered, such as –
- thickness of the restorative material,
- location of the restored tooth,
- patient occlusion and
- the vitality of the tooth
These play a role in choosing the type of restoration ie: Crown Vs Onlays.
The choice of different materials for indirect restorations has its own advantages and disadvantages. Ceramic onlays show enhanced longevity and esthetics when compared to composite ones which tend to wear. Indirect resin restorations, such as in this case on the other hand
- can be easily modified,
- can be easily polished
- require less removal of tooth structure resulting in further minimally invasive preparations.
Furthermore,
- these can be made chairside by the clinician
- no need of special equipment, training or laboratory support.
There are other chairside techniques apart from the one used in this case, where in fast setting epoxy resin dye can be used in place of stone dye for ease of fabrication and retrieval of the restoration. If the clinician is well versed with the techniques, then any can be used predictably.
Conclusion
Indirect chairside composite restorative technique is very useful in restoring large defects predictably. It also increases the longevity of the treatment and minimizes the stress to the clinician of rehabilitating the form and function of such severely compromised teeth.
















Comments