A new study published in the Journal of Science Translational Medicine suggests that periodontal disease results in repeated breaches of the oral mucosa that release citrullinated oral bacteria into circulation, which activate inflammatory monocyte subsets that are observed in inflamed RA synovia and blood of RA patients with flares.

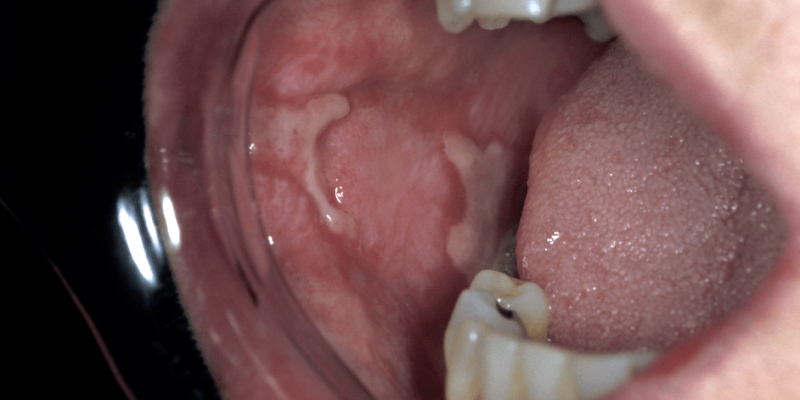
Periodontal disease is more common in individuals with rheumatoid arthritis (RA) who have detectable anti-citrullinated protein antibodies (ACPAs), implicating oral mucosal inflammation in RA pathogenesis.
Longitudinal blood samples from RA patients were taken and paired analyses of human and bacterial transcriptomics were performed. The results suggested that patients with RA and periodontal disease experienced repeated oral bacteremias associated with transcriptional signatures of ISG15+HLADRhi and CD48highS100A2pos monocytes, recently identified in inflamed RA synovia and blood of those with RA flares.
The oral bacteria observed transiently in blood were broadly citrullinated in the mouth, and their in situ citrullinated epitopes were targeted by extensively somatically hypermutated ACPAs encoded by RA blood plasmablasts.
The findings of this research may pave the way for more targeted therapies for RA sufferers.
Source: Science Translational Medicine















Comments