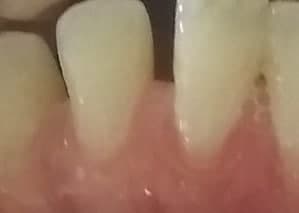
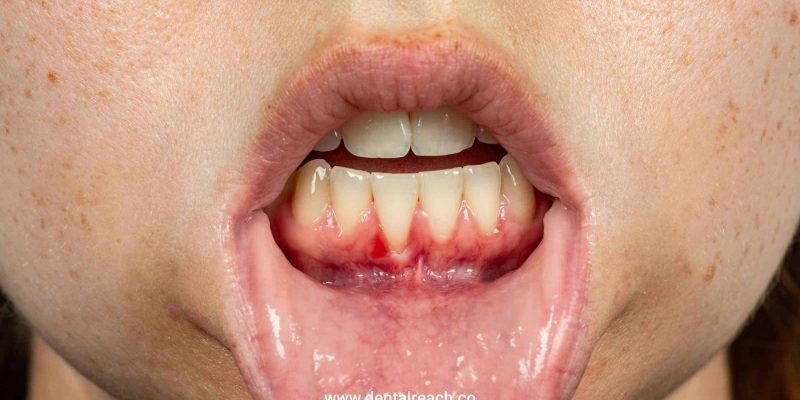
Normally, gingival margin is located at or coronal to cementoenamel junction (CEJ). When gingival margin migrates apical to CEJ, it is called a gingival recession. Gingival recession may occur due to excessive tooth brushing trauma. Localised plaque induced inflammatory process, malocclusion, and orthodontic tooth movement, as a part of generalised chronic periodontitis.
Treatment
For treating gingival recession it is important to diagnose the cause of recession. Elimination of causative factors is the most important step in treating recessions. This may include oral hygiene technique modifications, treating periodontitis, elimination of plaque retentive structures, tooth repositioning, etc.
After this, surgical intervention can be considered if the goal is to correct the defect and possible root coverage by regenerated gingiva.
Indications for Root Coverage
- Highly esthetic demands
- Lack of keratinised gingiva
- Continuous recession even after eliminating causative factors
- Root hypersensitivity
Connective Tissue Graft (CTG)
This technique utilises subepithelial CTG from the palate. Palate has keratinised tissue with dense lamina propria. The connective tissue grafting along with the various flap techniques can be used to treat recessions. The coronally advanced flap plus connective tissue grafting is still the gold standard in treating recessions.
Indications for CTG
- Inadequate tissue around recession defect
- Wide gingival recession defect
- Multiple gingival recessions
Advantages
- It has high predictability
- Graft receives abundant blood supply from the inside of the flap as well the periosteum- connective tissue
- Wound can be sutured at palatal donor site after harvesting of connective tissue graft. Which make hemostasis easy and healing rapidly.
- Less discomfort and pain during healing
- Better aesthetic results
- Multiple gingival recession defects can be treated.
Disadvantages
- Technically demanding
- As the graft is thick, the grafted tissue is thick. Gingivoplasty may require sometimes to obtain better morphology
Contraindications
If the thickness of donor tissue is less. The thickness of the connective tissue graft for root coverage should be 1.5-2.0 mm, and the thickness of the palatal flap should be 1.5-2.0 mm after graft harvesting, to prevent further necrosis. As a result, at least 3-mm thickness is required at the donor site of palatal soft tissue.
CTG Technique
- Local anaesthesia application
- Preparation of exposed root surface
- Recipient bed preparation
- CTG harvesting
- Suturing and stabilizing the graft at the recipient site
- Management of donor site
Preparation of the Exposed Root Surface
Scaling and root planning of the exposed root surface. If the goal is to obtain root coverage over existing caries or class V restoration, caries and restoration must be completely removed. Recent studies have shown root coverage over restored root surfaces too. Convexity of the root should be eliminated with diamond burs. Chemical root surface modifiers such as citric acid, tetracycline, EDTA is used to demineralise and decontaminate the root surface and to expose the collagen fibres. This is to facilitate attachment of fibres to the root surface. Evidence recently demonstrated that the use of such chemical modifiers provides no additional benefit of clinical significance. (Mariotti et al 2003).
Preparation of the recipient bed
The recipient bed is prepared for the connective tissue graft by a split thickness flap which is performed so as the periosteum remains attached to the underlying osseous structure. The split thickness flap is prepared by sharp dissection using 15 c blade. Presence of any muscle fibres or attachment is also eliminated so that flap is mobile and can be coronally repositioned without any tension.
Harvesting CTG from the Palate
The CTG is harvested from the hard palate area. The ideal location for harvesting the graft is 5-6 mm apical to the gingival margin of the palatal aspects of the maxillary premolars and the mesial half of the maxillary first molar. Incisions are made to gain access to the connective tissue. The incisions create a trap door effect where a flap is raised toward the palate, and then the connective tissue is harvested. There is different incision technique’s single incision, double incision, L- shaped incision. The ideal thickness of the graft is 1-1.5 mm thick. During harvesting, the connective tissue extra precautions should be taken to avoid injury to the vital structures like the greater palatine artery. Depending on the depth of the palatal vault, generally, the artery is about 12 mm apical to the gingival margin. Reiser et al 1996, Monnet-Corti et al 2006.
Placement of the Graft
The harvested connective tissue graft is immediately placed in the recipient site and secured into position with sutures. The 5-0 silk or 6-0 absorbable sutures can be used. Optimised healing requires the graft to be in intimate contact with the recipient bed with the absence of any dead space. Suturing techniques play an important role in the success of any periodontal plastic surgery.
Management of the Donor Site
For better healing, positive hemostasis is required at the donor site and can be achieved by application of pressure. Hemostatic agents like collagen sponges may be used to aid with hemostasis. Ligation of the greater palatine artery with a suture in case of injury to the artery. For patient comfort, dressing in the form of tinfoil may be placed or palatal stent that should be pre-surgically fabricated may be inserted.
Post-Operative Maintenance
Patient should be recalled for reassessment in between 2 weeks following surgery for a post-operative visit and suture removal better to use absorbable sutures. Patient should be instructed to avoid tooth brushing and flossing around the surgical site for first 2 weeks. Gentle rinsing with chlorhexidine gluconate 0.12% or 0.2 % should be advised.
Causes of CTG Failure
- Insufficient interdental bone and soft tissue heights
- If horizontal incision placed apical to the CEJ
- Reflection of interdental papilla
- Flap tearing
- Inadequate or improper root planing
- Failure to provide sufficient blood supply from surrounding tissue due to inadequate recipient site preparation is the main cause for failure
- CTG too small
- Graft too thick
- Failure to cover graft coronally by the flap
Conclusion
Management of gingival recession requires the identification and elimination of the etiology. Many recessions do not require treatment. In some cases, the decision may be to treat the recession with a root coverage procedure. One of the most predictable techniques is CTG.
Connective tissue grafting
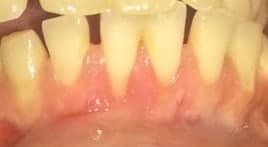
- Preoperative
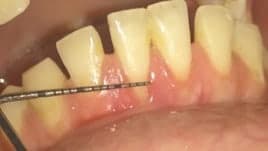
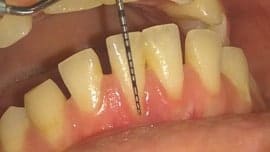
2. Incision and recipient bed preparation
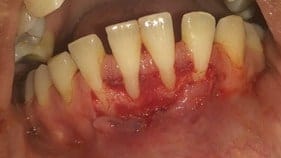
3.CTG Graftt
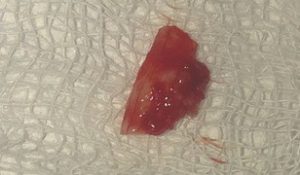
4.Donor site suturing
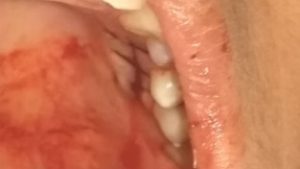
5. Graft stabilization
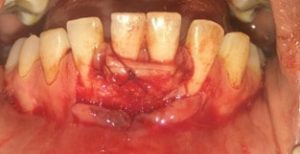
6. Flap suturing
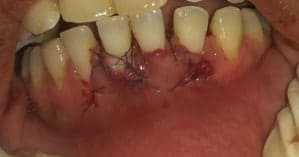
7. Results after 3 weeks


















Comments