Early childhood caries (ECC) affects one in two children below the age of 6 years in India.1 This is an alarming ratio and should call for immediate concern.
Preventive dentistry – the need of the hour
A disease with a 40% prevalence in children, who have a long life ahead of them, is considered a serious public health problem and requires focused attention. Caries management strategies primarily consist of:
- preventive treatment methods and
- non preventive treatment methods.
Preventive strategies aim to prevent the onset of caries and protect teeth from undesirable effects of caries. These include diet counseling, good oral hygiene, use of fluoridated tooth paste, application of pit and fissure sealants and sodium fluoride varnish.
Non preventive treatment methods involve arresting or slowing caries progression by mechanical caries removal and restoration of lost tooth structure.2
In 2014, 38% silver diamine fluoride (SDF) was approved by the FDA for use in children with ECC.3 SDF combines the antibacterial effects of silver and the remineralizing effects of fluoride and, is therefore a promising agent in both caries prevention as well as treatment.
What is Silver Diamine Fluoride (SDF)?
SDF (38% Ag (NH3)2F) is a clear liquid composed of 24-29% silver and 5-6% fluoride. It is alkaline at a pH of 10. Silver contributes to the antimicrobial effect and fluoride is responsible for the observed remineralization effect.2
First introduced in Japan in the 1960’s, it has been in use for more than 50 years to arrest dental caries in children.
An undesirable effect is its distinctive permanent black staining of teeth. Despite this drawback, American Academy of Pediatric Dentistry (AAPD) has concluded that 38% SDF is currently the best evidence-based material to arrest caries for children, adults, and patients with special needs.
Mechanism of action
SDF derives its effectiveness from silver nitrate and fluoride. The three significant mechanisms in arresting or preventing caries are 4–
- Antibacterial action on cariogenic bacteria (by silver)
- Remineralization and inhibition of demineralization of enamel and dentin (by fluoride) and
- Inhibition of dentin collagen type I degradation (by fluoride)
- Antibacterial action on cariogenic bacteria– Silver ions penetrate the lesion and exert their influence to about 25–30 microns into enamel, 200–300 microns into the dentin, and up to 2 mm into a deep carious lesion. Silver, due to its positively charged ions, adheres to the negatively charged bacterial cell wall and prevents bacterial aggregation. It has been hypothesized that silver interacts with bacterial enzymes, blocking the electron transport system, causing enzyme deactivation, membrane rupture and subsequently, cell death.
- Remineralization and inhibition of demineralization– SDF reacts with tooth hydroxyapatite and forms silver phosphate and calcium fluoride which promotes remineralization. Additionally, silver ions obturate dentinal tubules contributing to an increase in dentin hardness, which in turn makes the lesion cariostatic.
- Inhibition of dentin collagen type I degradation– The fluoride in SDF is proposed to have a potent inhibitory effect on the proteolytic enzymes, MMP-2, MMP-8, and MMP-9, reducing dentin collagen degradation in carious lesions.
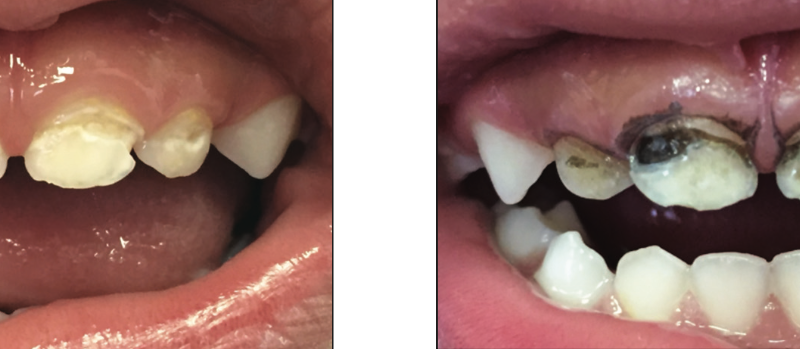
Mechanism of discoloration
Silver compounds such as silver oxide and silver phosphate are responsible for the permanent black staining of the carious lesions.4 (Figure 1) If soft tissues come into contact during application, the oral mucosa may be stained temporarily with henna-like discoloration. Since the dermis cannot absorb silver, the stains will disappear over about 14 days as the keratocytes are shed.3

Indications
- SDF is indicated in active carious lesions within dentin, without any clinical signs of pulp involvement.5 When possible, radiographs must be taken to assess depth of lesions.
- SDF can also be used prior to placement of restoration, as a part of caries control therapy.
Patients who benefit with application of SDF are those with
- High caries risk with active, cavitated carious lesions in anterior or posterior teeth
- Behavioral challenges and/or children with special healthcare needs when local or general anaesthesia is not possible
- Multiple cavitated caries lesions which would otherwise require multiple visits
- Cavitated dental caries lesions that are difficult to treat
- Difficult access to dental care
Contraindications
- Patients who are allergic to silver and
- those with spontaneous or nocturnal pain
are contraindicated from receiving SDF.
Clinical steps in the application of SDF
Obtain an informed consent from parents regarding permanent staining of teeth. Use of pictures, before and after SDF applications are recommended for better understanding.

Complete caries excavation is not necessary prior to application of SDF. It may be applied without or with minimal excavation, especially in children with limited co-operation. However, there are factors to consider- Dentinal staining will be more without excavation and with the presence of greater residual bacterial load and, caries arrest may take longer and more frequent applications may be required. 2 (Figure 2)

Follow up
Recall the patient after two to four weeks of initial treatment to check the arrest of the lesions treated. Additional SDF can be applied at recall appointments as needed, based on the color and hardness of the lesion or evidence of lesion progression. Post SDF, tooth can be restored with adhesive materials. When lesions are not restored after SDF therapy, bi- annual reapplication shows increased caries arrest rate versus a single application.
Safety and Adverse effects
Safety trials that have used it in more than 3800 individuals reported no serious adverse effects.6 Minor effects like:
- permanent black staining of teeth,
- metallic taste,
- pulpal and soft tissue irritation and
- development of small white reversible lesions in the oral mucosa
have been reported.
Effectiveness of SDF
The proportion of caries arrest on primary teeth treated with different application protocols (one time application, annual, biannual) was 81%. Anterior primary teeth showed higher rates of caries arrest than posterior primary teeth. Larger lesions and those with visible plaque had lesser likelihood of caries arrest. For children with poor oral hygiene, caries arrest rate can be increased by doubling the frequency of application from annually to semiannually.6
SDF versus Sodium fluoride (NaF) varnish
Studies reveal that teeth treated with SDF showed more arrested caries than those treated with sodium fluoride varnish. Chu et al compared bi annual application of 38% SDF with the application of 5% sodium fluoride varnish every 3 months in upper anterior teeth. After 30 months, all teeth treated with SDF showed arrested caries in comparison to only 66% of those treated with 5% NaF varnish.7
SDF versus Acidulated phosphate fluoride (APF) gel
Studies show that SDF arrests caries more effectively than acidulated phosphate fluoride gel. Shah et al assessed Streptococcus mutans counts in saliva after application of SDF and APF gel. After 12 months, there was no reduction in S. mutans counts in the APF gel group, while the SDF group showed significant reduction.
A study assesed the DMFS scores at 0, 6 and 12 months of application of SDF and APF gel in children. After 12 months, no new carious surfaces were observed in the SDF group, while two new carious surfaces in the APF gel group. The study concluded that SDF is a more effective caries arresting agent than APF.8
Convincing parents for SDF – Parent information note
Walking parents through any procedure for their child is an essential part of treatment planning. The primary concern with SDF is the black stain it produces, which needs to be emphasized with photographs showing the effect of SDF on teeth.
The below concise table will help you guide parents through their decision making on whether or not to use SDF.9

SDF – Black Magic!
SDF is an extremely effective caries arresting agent and must be considered as an alternative to sodium fluoride varnish and traditional tooth colored restorations when its benefits outweigh esthetic concerns. It can be the first line of treatment in
- very young children,
- in children fearful of dental treatment and
- in children with special healthcare needs.
Like any treatment, SDF has specific indications. Therefore the risk of permanent black tooth discoloration versus benefit of caries arrest must be considered before being offered to parents as a line of treatment.
References
1. Ganesh A, Muthu MS, Mohan A, Kirubakaran R. Prevalence of Early Childhood caries in India- A systematic review. Indian J Pediatric 2019; 86 (3) 276-86.
2. Trieu A, Mohamed A, Lynch E. Silver diamine fluoride versus sodium fluoride for arresting dentine caries in children: a systematic review and meta-analysis. Sci Rep 2019; 9 (1):2115
3. Khurshid Z, Shabbir J, Al Otaibi AK et al. Role of Silver Diamine Fluoride in dentistry. Eur Dent Res Biomater J 2020; 1:27-31
4. Nuvvula S, Mallineni SK. Silver Diamine Fluoride in Pediatric Dentistry. J South Asian Assoc Pediatr Dent 2019;2(2):73–80.
5. Crystal YO, Marghalani AA, Ureles SD, et al. Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent 2017;39 (5):E135-E145
6. Crystal YO, Niederman R. Evidence based dentistry update on silver diamine fluoride. Dent Clin North Am. 2019; 63(1): 45–68
7. Chu CH, Lo ECM, Lin HC. Effectiveness of silver diamine fluoride and sodium fluoride varnish in arresting dentin caries in Chinese preschool children. J Dent Res 2002; 81(11): 767-70
8. Gunasekaran S et al. Effectiveness of Silver diamine fluoride vs sodium fluoride and acidulated phosphate fluoride as a topical fluoride in caries prevention of primary teeth: A systematic review. Int J Dent Sci Inn Res 2019; 2 (6): 562-78
9. Horst JA, Ellenikiotis H, Milgrom PM. UCSF Protocol for Caries Arrest Using Silver Diamine Fluoride: Rationale, Indications, and Consent. J Calif Dent Assoc. 2016 January ; 44(1): 16–28
Author – Dr Divya Prahlad

















Comments