A 14 year old female patient from Moradabad, UP reported to the clinic in March, 2016.
Chief complaint- patient complained of intermittent pain in lower front tooth region since 6 months and missing teeth in upper front tooth region since 6 years.

History of present illness- patient was completely asymptomatic, till she met with an accident while playing 6 years back and got her upper and lower front tooth fractured for which she got treated by a nearby dentist. Then six months back she experienced intermittent pain in lower front tooth region. Pain was spontaneous, high intensity and got relieved on taking medicine.
Prenatal history – No relevant history of any illness or trauma during pregnancy was reported. No history of any drug therapy during pregnancy.
Natal history – The delivery was a full term, normal delivery. No history of jaundice or cyanosis at birth. No history of any blood transfusion was reported.
Post natal history
- Milestones Of Development: Normal
- Was She Immunized With Triple Vaccine : Yes
- Does She Have Frequent Minor Accidents Or Injuries? No
- Allergic To Any Food Or Drug? No
- Does She Have Brother/Sister? 4 Elder Sister And 1 Younger Brother.
- Past Medical History: No Relevant Medical History Reported.
- Past Dental History: 2nd Visit To A Dental Clinic.
- Oral Hygiene History – Brushing Once In A Day.
General physical examination
- Gait: No Abnormality Reported
- Body Type: Mesomorphic
- Posture: Erect
- Built: Athletic
- Height: 5 Feet
- Weight: 40 Kg
- Shape Of Head: Mesocephalic
- Facial Form: Oval
- Facial Symmetry: Bilaterally Symmetrical
- Facial Divergence: Straight
Extra oral examination
No abnormality detected in hairline, skin, eyes, nose, ears, lips, nails, Lymph Nodes and TMJ.

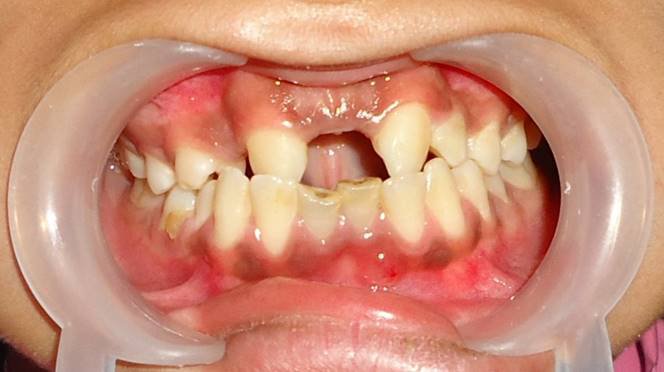
Intra oral examination
No abnormality was detected on the Mucosa, Palate, Floor of the Mouth, Tongue, Salivary Gland, Lymph Nodes.
Gingival swelling with sinus tract irt 31


Hard Tissue Examination
Teeth present- permanent dentition 17 16 15 14 13 23 24 25 26 27
47 46 45 44 43 42 41 31 32 33 34 35 36 37
Stains/Calculus- +/+ Abscess irt 31 T.O.P +Ve irt 31 32 41 42
Vestibular tenderness +ve irt 31 41 Root stump irt 85 Missing teeth irt 11 12 21 22
Molar relationship- Angle’s class I molar relation on right side .
Angle’s class II on left side.

Provisional diagnosis
Chronic apical periodontitis irt 32 42.
Chronic periapical abscess irt 31 41
Chronic irreversible pulpitis irt 85
Ellis class v irt 11 12 21 22
Investigations:
- Pulp vitality 32,42
- IOPAR irt 31,32,41,42
- Blood investigations were done.


Pulp vitality tests:
Heat test : There was no response irt 32 and 42
Final Diagnosis
Chronic periapical abscess irt 31 32 41 42 .
Chronic irreversible pulpitis irt 85
Ellis Class V fracture irt 11 12 21 22
Treatment plan:
- Emergency Phase : Access opening irt 32 42.
- Medical/Systemic Phase : Tab. Amoxicillin 500 mg B.D for 3 days, Tab Ibuprofen 400 mg S.O.S.
- Preventive Phase : Oral Hygiene Instructions given.
- Preparatory Phase : Oral Prophylaxis.
- Corrective Phase : Re-treatment of root canal treatment irt 31, 41 and access opening irt 32,42 followed by Apicoectomy irt 31 32 41 42 , extraction irt 85 and prosthetic rehabilitation will be done for missing teeth irt 11 12 21 22.
- Maintainence Phase : Periodic Recall And Follow Up every 3 months will be done.
- Surgical phase:

- Re-treament of root canal was done.
- After obturation with gutta percha and zinc oxide eugenol as a sealer, apicoectomy surgery was done the very next morning.
- Premedication with diazepam and antibiotic prophylaxis was done one night before the surgery.


Discussion
Apical surgery belongs to the field of endodontic surgery that also includes incision and drainage, closure of perforations, and root or tooth resections. The objective of apical surgery is to surgically maintain a tooth that has an endodontic lesion which cannot be resolved by conventional endodontic (re-) treatment.
This goal should be achieved by root-end resection, root-end cavity preparation, and a bacteria-tight closure of the root-canal system.
Indications:
1. Need for surgical drainage
2. Failed nonsurgical endodontic treatment
- Irretrievable root canal filling material
- Irretrievable intra-radicular post
3. Calcific metamorphosis of the pulp space
4. Procedural errors
- Instrument fragmentation
- Non-negotiable ledging
- Root perforation
- Symptomatic overfilling
5. Anatomic variations
- Root dilaceration
- Apical root fenestration
6. Biopsy
7. Corrective surgery
- Root resorptive defects
- Root caries
- Root resection
- Hemisection
- Bicuspidization
8. Replacement surgery
A) Replacement surgery
- Intentional replantation (extraction/replantation)
- Post-traumatic
B) Implant surgery
- Endodontic
- Osseointegrated
Contraindication:
- Inadequate periodontal support and active uncontrollable periodontal disease.
- Presence of systemic diseases—leukaemia, uncontrolled diabetes, anaemia, thyrotoxicosis, etc.
- Teeth damaged beyond restoration
- Traumatic occlusion
- Poor root crown ratio
- Acute infection which is nonresponsive to the treatment
- Anatomic structures (e.g., adjacent nerves and vessels)
PROCEDURE:
Full mucoperiosteal Incision
- The full mucoperiosteal incision is made into the gingival sulcus, extending to the gingival crest. This procedure includes elevation of interdental papilla, free gingival margin, attached gingiva, and alveolar mucosa.
- Two vertical releasing incisions may be used, creating a rectangular design or trapizoidal design.
The full mucoperiosteal design is preferred over the other techniques.
The advantages include maximum access and visibility, not incising over the lesion or bony defect, allowance of root planing and bone contouring, and reduced likelihood of healing with scar formation.
The disadvantages are that the flap is more difficult to replace and to suture; also, gingival recession can develop if the flap is not reapproximated well, exposing crown margins or cervical root surfaces.
USE OF GRAFT MATERIAL:
Bone graft material includes autogenous graft, allograft, xenograft, ceramic/synthetic grafts, bioactive proteins, combination graft.
Platelet rich fibrin can be used as an autologous biomaterial after an endodontic surgery. This is second generation platelet concentrate. It was first developed in France by Choukroun et al. in 2001.
This is widely used in stimulation and acceleration of soft tissue and bone healing because of local and continuous delivery of growth factors and proteins, mimicking the needs of the physiological wound healing and reparative tissue processes.
The growth factors which are released from activated platelets are:
- Platelet derived growth factor(PDGF)
- Transforming growth factors beta 1 and beta 2 (TGF 2. β 1 & 2)
- Vascular Endothelial Growth Factor (VEGF
- Platelet derived endothelial cell growth factor
- Interleukin – 1 (IL-1), Basic fibroblast growth factor (bFGF)
- Platelet activating factor -4 (PAF-4) .
Singh et al in 2013 conducted a study in which 15 cases were presented with conventional endodontic therapy failure in resolving the problem and periapical root – end surgery was required. At the end of six months, all patients showed complete bone regeneration. They concluded that the production of a dense, cross – linked, physically robust PRF made of intact platelets and fibrin by high speed centrifugation in the absence of exogenous thrombin, yields an ideal scaffold for use in tissue repair.
Newer Materials:
Platelet Rich Fibrin and Nanocrystalline Hydroxyapatite with Collagen Combination.
The PRP and Hydroxyapatite combination facilitated better and faster bone regeneration when compared to PRP alone.
Group 1– hydroxyapatite- 1year
Group 2 – prp- 9 months
Group 3– prp +hydroxyapatite- 6 months
CONCLUSION:
Apical surgery is now considered a predictable treatment option to save a tooth with apical pathology that cannot be managed by conventional, non-surgical endodontics.
REFERENCES:
- Kenneth M. Hargreaves, Stephen Cohen. Cohen’s pathways of the pulp. 10th edition: 2011.
- Chandra BS, Krishna VG. Grossman’s endodontic practice. 12th edition: 2012.
- Singh S, Singh A, Singh R. Application of PRF in surgical management of periapical lesions. Natl J Maxillofac Surg. 2013; 4(1): 94-99.
- Apical surgery: A review of current techniques and outcome. Thomas von Arx. The Saudi Dental Journal (2011) 23, 9–15
- Vaishnavi C, Mohan B, Narayanan L. Treatment of endodontically induced periapical lesions using hydroxyapatite, platelet-rich plasma, and a combination of both: An in vivo study. J Conserv Dent. 2011:14(2);140-144.


















Comments