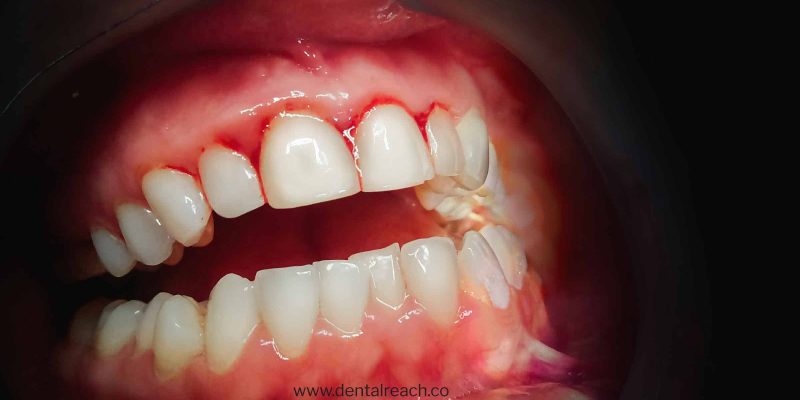
Bleeding on probing is also known as bleeding gums or gingival bleeding. It is a term used by dentists and dental hygienists when referring to bleeding that is induced by gentle manipulation of tissues at the depth of the gingival sulcus. Bleeding on probing, abbreviated as ‘BOP’ is an objective, easily assessed and widely used criterion to diagnose gingival inflammation.
The two earliest signs of gingival inflammation are:
- Increased gingival crevicular fluid production rate
- Bleeding from gingival sulcus on gentle probing
Bleeding on probing appears as a change in colour or other visual signs of
inflammation. Gingival bleeding on probing indicates an inflammatory lesion
both in epithelium lining of the sulcus and in the connective tissue. The blood
comes from lamina propria after ulceration of the lining.
Peer-reviewed dental literature thoroughly establishes that bleeding on probingis a poor positive predictor of periodontal disease, but conversely, lack ofbleeding is a strong negative predictor. The clinical interpretation of thisresearch is that BOP presence may not indicate periodontal disease, the
continued absence of BOP is a strong predictor (approximately 98%) of
continued periodontal health.
Local Factors Associated With Bleedingon Probing
There are many possible causes of gingival bleeding. The main cause of gingival bleeding is the formation and accumulation of plaque around the teeth due to improper brushing and flossing of teeth. The hardened or calcified form of plaque and calculus provides an ideal surface for further plaqueformation. Contributing factors to plaque retention may lead to gingivitis and ultimately lead to gingival bleeding on probing. The contributing factors include caries, malpositioned teeth, mouth breathing, partial dentures, lack of attached gingiva and fixed orthodontic treatment.
Chronicand Recurrent Bleeding
Most common cause of gingival bleeding is gingival inflammation. Bleeding is chronic and provoked by mechanical trauma. Bleeding may occur from tooth brushing, toothpicks and food impaction. It may also occurby biting into solid food such as apples. Traumatic injuries such as laceration of gingiva by toothbrush bristles during aggressive tooth brushing or by sharp pieces of hard food can cause gingival bleeding even in the absence of gingival disease. Gingival burn from hot food and chemical increase the chances of gingival bleeding. Spontaneous bleeding or bleeding on slight provocation can occur in Acute Necrotizing Ulcerative Gingivitis (ANUG).
Histological evaluation has revealed that in early stages of gingivitis, cytokines are responsible for connective tissue breakdown. Matrix metalloproteinase also plays a vital role in tissue breakdown. Histopathologic alterations that result in abnormal gingival bleeding include dilatation & engorgement of the capillaries, & thinning or ulceration of the sulcular epithelium. After the vessels are damaged & ruptured interrelated mechanisms induce hemostasis. Vessel wall contract, blood flow diminishes, blood platelets adhere to the edges of tissue and a fibrous clot is formed, which contracts & results in approximation of edges of the injured area. Bleeding recurs when the area is irritated. In case of moderate or advanced periodontitis, the presence of bleeding on probing is a sign of active tissue destruction.
Systemic Factors
Hemorrhagic disorders in which abnormal gingival bleeding is encountered include:
- Vitamin C deficiency (scurvy): Interdental & marginal gingiva is bright red with swollen, smooth and shiny surface. In fully developed scurvy, gingiva becomes boggy, ulcerated and bleeds spontaneously.
- Platelet disorders (thrombocytopenic purpura): There is an abnormal reduction in number of circulating blood platelets so patient develops focal haemorrhage into tissue & organs, including skin & mucous membrane.
- Vitamin K deficiency: It is involved in prothrombin synthesis. It also regulates the level of factor VII, IX & X (proconvertin, christmas factor & stuart-prower factor, respectively). Hence, its deficiency leads to gingival bleeding.
- Other coagulation defects:
- Haemophilia:It is characterized by prolonged coagulation time & haemorrhagic tendencies. Gingival haemorrhage in such cases may be massive & prolonged.
- Leukaemia:There is progressive overproduction of white blood cells which usually appear in circulating blood in an immature form. Oral manifestations are gingivitis, gingival hyperplasia, haemorrhage & ulceration of the mucosa.
- Christmas disease:It is also known as Haemophilia B, in which there is deficient level of coagulant factor IX (Christmas factor).
- The effect of hormonal replacement therapy, oral contraceptives, pregnancy & the menstrual cycle are also reported to affect the gingival bleeding.
- Diabetes:Marked inflammation noted in diabetic patients affects both epithelium & connective tissue which leads to destruction of reticulin fibers. The low immunity also makes them susceptible to opportunistic infections like candidiasis.
- Medications: Anticonvulsants, antihypertensives & immunosuppressants are well known to cause gingival enlargement and increases the susceptibility of gingival bleeding.
Diagnosis
In order to determine the periodontal health of a patient, the sulcular depths of gingiva needs to be recorded followed by observation of any bleeding on probing. This is often accomplished with the use of a periodontal probe. A periodontal probe is a calibrated probe used to measure the depth and determine the configuration of a periodontal pocket. The insertion of probe to the bottom of the pocket elicits bleeding if the gingiva is inflamed & the pocket epithelium is atrophic or ulcerated. The probe is carefully introduced to the bottom of the pocket for bleeding test & gently moved laterally along the pocket wall. Sometimes bleeding appears immediately after removal of the probe; other times it may be delayed for few seconds. Therefore, recheck for bleeding on probing after 30 to 60 seconds.
An examination to rule out the systemic factors contributing to gingival bleeding helps to formulate the appropriate patient management protocol. Additional corresponding diagnosis tests to certain disease may be required. This includes oral glucose tolerance test for diabetes mellitus, blood studies, human gonadotrophin levels for pregnancy, radiologic imaging for teeth and jaw bones.
Alternatively, a dental floss may also be used to assess the gingival bleeding index. It is used as an initial evaluation of patient’s periodontal health especially to measure gingivitis. The number of bleeding sites is used to calculate the gingival bleeding score.
Many bleeding indices have been devised; some assess bleeding as simply present or absent, whereas others use grading in an attempt to assess severity of bleeding. The choice of which index to use depends on whether the purpose is an epidemiological survey, a clinical study, diagnosis and treatment. Bleeding may be elicited manually with toothpicks, dental floss and a periodontal probe. A controlled-force probe may be expensive and can cause less trauma and false-positive bleeding from healthy tissues.
There is evidence that smokers have less or delayed gingival bleeding when compared with non-smokers. Therefore smoking needs to be controlled to avoid gingival bleeding. Measurement of gingival bleeding tendency should be an integral part of a comprehensive oral examination. In clinical practice, the use of graded bleeding index is more likely to identify sites that are at risk of further destructive activity. Hence, bleeding indices are good tools for monitoring individual patients both for initial therapy and maintenance.
Bleeding point index
It is used for the evaluation of gingival inflammation. Retract the cheek & place the periodontal probe 1mm into the sulcus or pocket at the distal aspect of posterior tooth in the quadrant for recording the index. Carry the probe lightly across the length of sulcus to the mesial interproximal area on the facial aspect. Wait for 30 seconds & record the presence of bleeding on the distal, facial & mesial surface. Repeat the same for palatal surface. Percentage of the number of bleeding surfaces is calculated by dividing the number of surfaces that bled by the total number of tooth surfaces (4 per tooth) and multiplied by 100. A score of 10% or fewer bleeding points are considered good but 0 is ideal.
Sulcus Bleeding Index (SBI)
Developed by Muhlemann HR and Sen S in 1971. It is a modification of Papillary-Marginal Index of Muhlemann and Mazor ZS.
Scoring Criteria:
- Score 0: Healthy looking papillary and marginal gingiva
- Score 1: Healthy looking gingiva, bleeding on probing
- Score 2: Bleeding on probing, change in colour, no edema
- Score 3: Bleeding on probing, change in colour, slight edema
- Score 4: Bleeding on probing, change in colour, obvious edema
- Score 5: Spontaneous bleeding, change in colour, marked edema
Four gingival units are scored systematically for each tooth include labial, lingual marginal gingival (M units) and mesial, distal papillary gingival (P units). Scores for these units are added and divided by four to determine the sulcus bleeding index.
Gingival Bleeding Index (GBI)
In 1947, Carter and Barnes introduced Gingival Bleeding Index, which records the presence or absence of gingival inflammation. The mouth is divided into six segments and flossed in the following order: upper right, upper anterior, upper left, lower left, lower anterior and lower right. However, 30 seconds is allowed for re-inspection of each segment. Bleeding is recorded as present or absent. For each patient, a gingival bleeding score is obtained by noting the total units of bleeding. Gingival bleeding index by Ainamo & Bay (1975) is performed through gentle probing of gingival crevice’s orifice.
Papillary Bleeding Index
This index was introduced by Saxer and Muehlemann in 1975. A periodontal probe is inserted into the gingival sulcus at the base of the papilla on mesial aspect and then moved coronally to the papilla tip. This is repeated on the distal aspect of the papilla. The intensity of any bleeding is recorded as:
- Score 0: No bleeding
- Score 1: A single discreet bleeding point
- Score 2: Several isolated bleeding points or a single line of blood appears
- Score 3: The interdental triangle fills with blood shortly after probing
- Score 4: Profuse bleeding occurs after probing, blood flows immediately into the marginal sulcus
Eastman Interdental Bleeding Index (EIB)
Caton & Polson developed this index in 1985. A wooden interdental cleaner is inserted between the teeth from the facial aspect, depressing the interdental tissues 1 to 2 mm. This is repeated four times and the presence or absence of bleeding within 15 seconds is recorded. Path of insertion should be parallel to occlusal surface. Insertion and removal of interdental cleaner are done four times and then moved on to next interproximal area.
Score = Number of bleeding areas/Total number of areas x 100
Treatment
- Mechanical plaque removal
- Corresponding treatments for diagnosed diseases must be given priority
- Dentists may prescribe soft-bristle toothbrush for brushing
- Flossing twice a day can prevent building up of plaque interdentally
- Tobacco should be avoided as it may aggravate bleeding gums
- Balanced healthy diet must be consumed
If there is persistent continuation of inflammation and bleeding, a prescription of antiplaque rinse would be useful.
Conclusion
BOP indicates the progression of attachment loss. If periodontal treatment is successful, bleeding on probing will cease. BOP is extremely important because it’s a wake-up call that gives the patient an opportunity to avoid a chronic and incurable disease. We have to heed signs and turn the patient around at this point for better health.
References
- Charles R. Craig, Robert E. Stitzel (2004) In Modern Pharmacology with clinical applications (Edition 6). Lippincott Williams & Wilkins. p. 506.
- Carranza’s Clinical Periodontology, 9th edition, 2002. page 447
- Hayes EB, Gubler DJ. Pediatr Infect Dis J 1992; 11: 311- 317.
- Absence of bleeding on probing. An indicator of periodontal stability. J Clin Periodontol 1990 Nov; 17 (10):714-21.
- Newbrun E. Indices to measure gingival bleeding. J Periodontol 1996 Jun; 67 (6):555-61.
Bonus: Download our monthly e-bulletin!Click here to get it
DISCLAIMER : “Views expressed above are the author’s own.”

















Comments